
Tanning Beds Psoriasis
In the pursuit of managing psoriasis, a chronic skin condition characterized by red, itchy, and scaly patches, patients and healthcare providers alike are constantly on the lookout for effective treatment options. Among the myriad of therapies available, one method to treat psoriasis that has sparked both interest and debate is the use of tanning beds. This article delves into the role of tanning beds in psoriasis management, exploring why tanning beds increase their potential benefits and improve psoriasis,, risks, and how they compare to other treatments to manage psoriasis, including an emerging therapy known as Red Light Therapy.
Psoriasis affects millions worldwide, not just physically but also emotionally and psychologically, making the quest for an effective treatment all the more critical. As we explore the use of tanning beds for psoriasis, it's important to approach the topic with an open mind, armed with knowledge and understanding of both the science and the personal experiences that shape our perspectives on this controversial treatment option.
Understanding Psoriasis
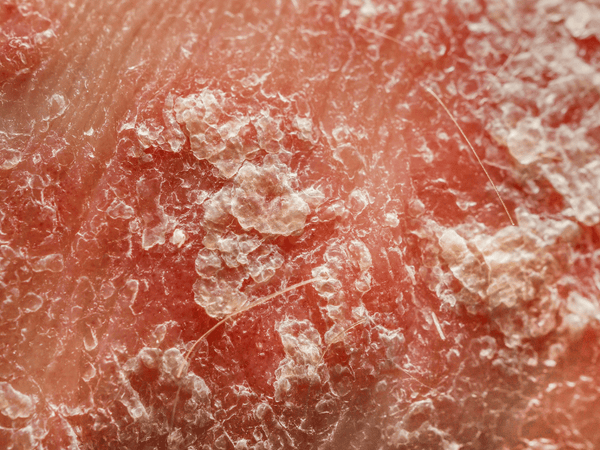
Psoriasis is a long-term autoimmune disorder that causes skin cells to divide more quickly, accumulating more cells on the skin's surface. This buildup and skin damage result in the formation of red, scaly patches of damaged skin that can be itchy, painful, and, at times, embarrassing for those affected. Psoriasis can appear anywhere on the body but is most commonly found on the scalp, elbows, knees, and lower back.
Types of Psoriasis
Psoriasis comes in various forms, each with its own set of characteristics:
-
Plaque Psoriasis: is the most common type, characterized by raised, red patches covered with a silvery-white buildup of dead skin cells.
-
Guttate Psoriasis: Typically seen in children and young adults, this form appears as small, dot-like lesions.
-
Inverse Psoriasis: found in the armpits, groin, and under the breasts, this type causes smooth patches of red, inflamed skin.
-
Pustular Psoriasis: is a rare form that causes pus-filled blisters on the skin.
-
Erythrodermic Psoriasis: is the least common type, characterized by a red, peeling rash that can cover the entire body.
Symptoms and Triggers
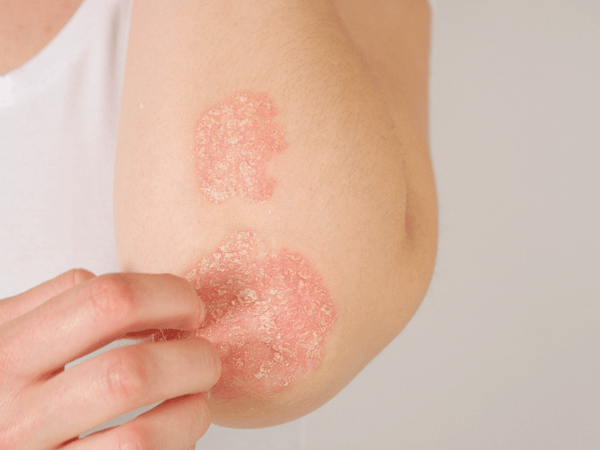
Psoriasis symptoms can vary from person to person but often include:
-
Red patches of skin covered with thick, silvery scales
-
Dry, cracked skin that may bleed
-
Itching, burning, or soreness
-
Thickened, pitted, or ridged nails
-
Psoriasis can be triggered by various factors, including:
-
Infections, such as strep throat
-
Skin injuries, such as cuts, scrapes, or sunburns
-
Stress
-
Smoking
-
Heavy alcohol consumption
Psychological Impact
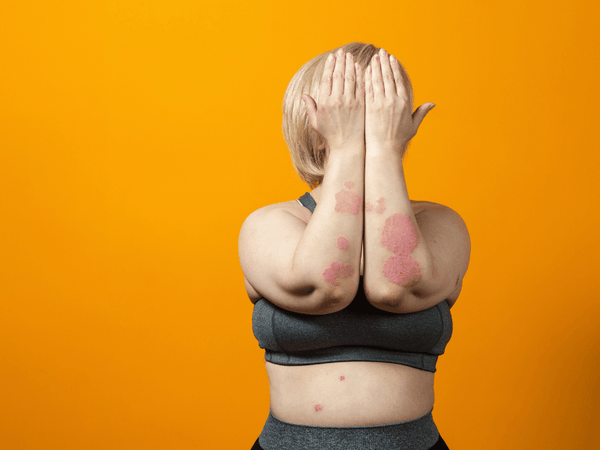
The impact of psoriasis goes beyond the physical symptoms. Many individuals with psoriasis experience emotional and psychological distress, including feelings of shame, embarrassment, and social isolation. The visible nature of the condition can lead to self-esteem issues, anxiety, and depression.
Traditional Treatments for Psoriasis
Managing psoriasis involves a multi-faceted approach, combining medication, lifestyle changes, and sometimes even psychological support. Here's an overview of the traditional treatments commonly used to alleviate the symptoms of psoriasis:
Topical Treatments
These are applied directly to the skin and are usually the first line of defense for mild to moderate psoriasis:
-
Corticosteroids: Reduce inflammation and relieve itching.
-
Vitamin D Analogues: Slow down the growth of skin cells.
-
Retinoids: Help to normalize skin cell growth.
-
Coal Tar: Reduces scaling, itching, and inflammation.
-
Moisturizers: Relieve dryness and soothe irritated skin.
Phototherapy (Light Therapy)
Exposure to ultraviolet (UV) light can cause skin damage and slow the growth of skin cells:
-
UVB Phototherapy: Treats moderate to severe psoriasis by exposing the skin to UVB light.
-
Psoralen Plus UVA (PUVA): Combines a light-sensitizing medication (psoralen) with UVA light exposure.
-
Excimer Laser: Targets specific areas of the skin with a high-intensity beam of UVB light.
Systemic Medications
For more severe cases, oral or injected medications that affect the whole body may be prescribed:
-
Methotrexate: slows the growth of skin cells and suppresses inflammation.
-
Cyclosporine: Suppresses the immune system to reduce symptoms.
-
Biologics: Target specific parts of the immune system to block the overactive response that leads to inflammation.
Lifestyle Changes
Apart from pharmaceutical interventions, alterations in lifestyle can be quite significant in the management of psoriasis:
-
Stress Management: Techniques like meditation, yoga, and counseling can help reduce stress, a known trigger for psoriasis flare-ups.
-
Diet: Some people find that certain foods exacerbate their symptoms. A balanced diet rich in anti-inflammatory foods may be beneficial.
-
Exercise: Regular physical activity can improve overall health and reduce the risk of comorbidities associated with psoriasis.
Tanning Beds as a Treatment Option

In the quest for effective psoriasis treatments, some individuals turn to tanning beds as an alternative or supplement to traditional therapies. Tanning beds emit ultraviolet (UV) light, which can have a therapeutic effect on psoriasis lesions. However, this approach to using ultraviolet light to treat psoriasis is not without controversy and requires careful consideration.
How Tanning Beds Work
Tanning beds use fluorescent bulbs to emit UV radiation, primarily in the form of both UVA rays and UVB rays. In the context of psoriasis treatment, the UVB component of ultraviolet light is of particular interest, as it can help slow the rapid growth of skin cells and reduce inflammation. This is similar to the principle behind conventional phototherapy treatments used in dermatology clinics.
The Rationale for Using Tanning Beds
The appeal of tanning beds for some psoriasis sufferers lies in their accessibility and convenience. Not everyone has easy access to a dermatologist or a specialized phototherapy clinic, making tanning beds an attractive option. Additionally, the warmth and light of tanning beds can provide a sense of relaxation and well-being.
Research and Studies
Several studies have explored the use of tanning beds for psoriasis treatment, with mixed results. Some research indicates that regular use of tanning beds can lead to improvement in psoriasis symptoms for certain individuals. However, it's important to note that these studies often involve specific types of tanning beds and controlled sun exposure and times, which may not reflect the conditions of typical tanning bed use or salon visits.
Considerations for Using Tanning Beds

-
Skin Cancer Risk: Prolonged exposure to UV radiation, whether from the sun or tanning beds, increases the risk of skin cancers, including melanoma.
-
Skin Aging: UV exposure can accelerate skin aging, leading to premature wrinkles and age spots.
-
Regulation and Control: Tanning beds in salons may not be regulated or calibrated specifically for psoriasis treatment, making it challenging to control the dose of UV exposure.
-
Individual Response: As with other psoriasis treatments, the effectiveness of tanning beds can vary from person to person.
Risks and Considerations

While indoor tanning beds may offer potential benefits for some psoriasis sufferers, it's essential to weigh them against the significant risks associated with their use. Here are some key considerations to keep in mind with indoor tanning beds:
Potential Risks
-
Skin Cancer: The most serious risk of tanning bed use is an increased likelihood of developing skin cancer, including melanoma, squamous cell carcinoma, and basal cell carcinoma. UV radiation damages the DNA in skin cells, which can lead to mutations and cancerous growths.
-
Premature Aging: UV exposure from tanning beds can lead to premature aging of the skin, characterized by wrinkles, age spots, and a leathery texture.
-
Burns: Overexposure to UV light can cause sunburn, which can be particularly painful and damaging for individuals with psoriasis.
The Importance of Moderation
If indoor tanning beds are used for psoriasis treatment, it's crucial to do so in moderation and under the guidance of a healthcare professional. Controlled, short-session indoor tanning beds that minimize the risk of burns and overexposure are essential.
Professional Guidance
Consulting with a dermatologist or healthcare provider is vital before starting any tanning bed treatment for psoriasis. They can provide personalized advice based on the doctor's supervision, severity of the condition, skin type, and overall health.
Alternatives to Tanning Beds
Considering the serious risks here, exploring alternative treatments for psoriasis is advisable. Phototherapy under medical supervision, topical treatments, systemic medications, and lifestyle changes can all be effective without the added risks of tanning beds ultraviolet radiation.
Preparing for Tanning Bed Therapy
If you and your healthcare provider decide that tanning bed therapy is a suitable option for managing your psoriasis, there are several steps you should take to prepare and ensure the treatment is as safe and effective as possible.
1. Consultation with a Dermatologist
-
Before starting any tanning bed therapy, consult with a dermatologist to discuss your psoriasis treatment plan and how tanning beds fit into it.
-
Your dermatologist can provide guidance on the frequency and duration of tanning bed sessions that are appropriate for your condition.
2. Choosing the Right Tanning Bed
-
Not all tanning beds are created equal. Look for a tanning bed that emits a higher proportion of UVB rays, as these are more effective for psoriasis treatment.
-
Some tanning salons offer beds specifically designed for psoriasis therapy. Inquire about these options.
3. Setting the Correct Exposure Time
-
Start with short sessions (e.g., 5-7 minutes) to see how your skin reacts and gradually increase the time as recommended by your healthcare provider.
-
Avoid overexposure, as this can lead to burns and increase the risk of skin cancer.
4. Protecting Healthy Skin
-
Apply a broad-spectrum sunscreen to areas of your skin that are not affected by psoriasis to protect them from unnecessary UV exposure.
-
Wear protective eyewear to shield your eyes from UV rays.
5. Monitoring Your Skin's Response
-
Keep track of any changes in your psoriasis symptoms and note any adverse reactions to the tanning bed therapy.
-
Regularly assess your skin for signs of overexposure, such as redness, burning, or new lesions.
6. Regular Check-ups
-
Schedule regular follow-up appointments with your dermatologist to monitor your progress and adjust your treatment plan as needed.
Red Light Therapy as an Alternative
In recent years, Red Light Therapy (RLT) has emerged as a promising alternative treatment for various skin conditions, including psoriasis. Unlike traditional UV-based therapies, RLT uses low-level wavelengths of red and near-infrared light to penetrate the skin and promote healing.
How Red Light Therapy Works
-
RLT devices emit red and near-infrared light, which is absorbed by the skin's mitochondria, the energy-producing organelles in cells.
-
This absorption stimulates the production of adenosine triphosphate (ATP), enhancing cellular energy and promoting repair and regeneration.
-
RLT is believed to reduce inflammation, increase collagen production, and improve skin texture and tone.
Benefits of Red Light Therapy for Psoriasis
-
Reduced Inflammation: RLT can help reduce the inflammation associated with psoriasis, leading to a decrease in the severity of plaques.
-
Improved Healing: By promoting cellular regeneration, RLT can accelerate the healing of psoriatic lesions.
-
Minimal Side Effects: RLT is non-invasive and has minimal side effects, making it a safe option for many individuals.
How to Use Red Light Therapy

-
RLT can be administered in a dermatologist's office or at home using a portable RLT device.
-
Treatment typically involves exposing the affected areas to red light for a specified duration, usually ranging from a few minutes to half an hour, depending on the device and the severity of the condition.
-
Consistency is key, with most protocols recommending several sessions per week for optimal results.
Considerations and Precautions
-
While RLT is generally considered safe, it's important to follow the manufacturer's instructions and consult with a healthcare professional before starting treatment.
-
Protect your eyes during RLT sessions, as direct exposure to intense light can be harmful.
Making an Informed Decision
Choosing the right treatment for psoriasis involves careful consideration of various factors. Here's a guide to help you make an informed decision:
Assessing Your Psoriasis
-
Severity: The extent and severity of your psoriasis will influence the choice of treatment. Mild cases may be managed with topical treatments, while more severe cases may require systemic medications or light therapy.
-
Location: The location of psoriasis plaques can affect treatment options. For example, scalp psoriasis might respond well to light therapy, while inverse psoriasis in sensitive areas may require gentler treatments.
-
Impact on Quality of Life: Consider how psoriasis affects your daily life, including your emotional well-being. Treatments that offer psychological benefits, such as Red Light Therapy, might be particularly valuable.
Evaluating Treatment Options
-
Effectiveness: Research the effectiveness of different treatments for your type of psoriasis. Look for clinical studies and patient testimonials.
-
Risks and Side Effects: Understand the potential risks and side effects associated with each treatment. Weigh these against the potential benefits.
-
Accessibility and Convenience: Consider the availability and convenience of the treatment. Tanning beds might be more accessible than a dermatologist's office, but they come with their own risks.
Consulting with Healthcare Professionals
-
Dermatologist's Advice: Always consult with a dermatologist or healthcare provider before starting any new treatment. They can provide personalized recommendations based on your medical history and condition.
-
Second Opinions: If you're unsure about a treatment plan, don't hesitate to seek a second opinion from another healthcare professional.
Making the Decision
-
Personal Preferences: Ultimately, the decision should align with your personal preferences and lifestyle. Choose a treatment that you feel comfortable with and can commit to consistently.
-
Monitoring and Adjusting: Be prepared to monitor your response to the treatment and adjust as necessary. Open communication with your healthcare provider is key.
Making an informed decision about psoriasis treatment requires a comprehensive understanding of your condition, the available options, and the potential risks and benefits. By taking a proactive and informed approach, you can find a treatment plan that works best for you.
FAQ Section
Q1: Can tanning beds cure psoriasis?
A: Tanning beds are not a cure for psoriasis. They may temporarily alleviate symptoms for some individuals, but they do not address the underlying causes of the condition.
Q2: How often should I use a tanning bed for psoriasis treatment?
A: The frequency of sun exposure and tanning bed sessions should be determined by a healthcare professional. Generally, starting with short, infrequent natural sunlight exposure sessions and gradually increasing as recommended is advisable.
Q3: Are there any specific types of tanning beds that are better for psoriasis treatment?
A: Tanning beds that emit a higher proportion of UVB rays natural sunlight are considered more effective for treating psoriasis than treatment. Consult with a dermatologist to find a suitable option.
Q4: Can red light therapy be used alongside other psoriasis treatments?
A: Yes, red light therapy can often be used in conjunction with other treatments. However, it's important to discuss your treatment plan with a healthcare professional to avoid any potential interactions.
Q5: How long does it take to see results from red light therapy for psoriasis?
A: Results from red light therapy can vary. Some individuals may notice improvements within a few weeks of laser therapy, while others may take longer. Consistency and adherence to the treatment protocol are key.
Q6: Is red light therapy safe for all skin types?
A: Red Light Therapy is generally considered safe for most skin types. However, individuals with certain skin conditions or sensitivities should consult with a healthcare professional before starting treatment.
Q7: Can lifestyle changes help manage psoriasis?
A: Yes, lifestyle changes such as stress management, maintaining a healthy diet, and regular exercise can help manage psoriasis symptoms and improve overall well-being.
Q8: Are there any natural remedies for psoriasis?
A: While natural remedies like aloe vera, oatmeal baths, and tea tree oil can provide temporary relief for some symptoms, it's important to consult with a healthcare professional before incorporating them into your treatment plan.
Conclusion
Psoriasis is a complex and chronic skin condition that requires careful management and a personalized treatment approach. While traditional treatments like topical medications and phototherapy remain the cornerstone of psoriasis management, alternative options like tanning beds and Red Light Therapy have gained attention for their potential benefits.
Tanning beds, though accessible and sometimes effective, carry significant risks, including an increased risk of skin cancer and premature aging. It's essential to approach this treatment option with caution and under the guidance of a healthcare professional.
Red Light Therapy, on the other hand, offers a safer alternative with promising results in reducing inflammation and promoting healing. Its non-invasive nature and minimal side effects make it an attractive option for many psoriasis sufferers.
Ultimately, the decision to pursue any further treatment for psoriasis should be made in consultation with a dermatologist or healthcare provider, taking into account the severity of your psoriasis, your overall health, and your personal preferences. By staying informed and proactive in your treatment plan, you can improve your quality of life and manage your psoriasis more effectively.

